Pure HealthyBack and Blue Care Network of Michigan
Functional Restoration Return On Investment Report April 4, 2015


Measurement Period: November 2, 2013 through May 31, 2015
Report Delivery: August 4, 2015
Introduction
Pure HealthyBack is a health management solution for people with chronic back or neck pain. The Pure Solution provides a clinic-based, physician-driven, and patient-centric approach that is redefining the way chronic back and neck pain is treated. PHB’s innovative and comprehensive care is delivered by expert teams comprised of highly qualified physicians, physical therapists, physical therapy assistants, exercise physiologists, health and wellness coaches, massage therapists, and yoga instructors all working together to implement our leading-edge treatment model—one that provides better care for individuals, improved health for the population, and reduced costs.
Claims-Based Results
Pure HealthyBack improves clinical outcomes and lowers avoidable utilization by addressing the critical interplay between chronic pain and overall physical health. Chronic pain conditions negatively impact quality of life and functionality, and they also impede adherence to all prescribed treatment plans and preclude optimal physiologic response to various treatment modalities. Effective identification and management of targeted patients result in overall reductions in health care services and associated costs.
PHB contracted with Blue Care Network of Michigan (BCN) to serve program-eligible patients identified through the PHB identification process, which is described below. This report presents the financial savings with complete data sets either equal to or exceeding 12 months of post-period utilization and costs for all BCN patients beginning in November 2013 and concluding at the end of May 2015.
PHB Identification
Critical to program success is the identification of members who represent the greatest opportunity for change and impact. Through the collaborative PHB identification process, patients are selected using proprietary data analytics in combination with agreed upon inclusion/exclusion criteria. Health care claims and membership enrollment data are used to determine presence and severity of condition and eligibility for program enrollment, as well as financial performance and clinical outcomes over time.
Return on Investment
Return-on-Investment (ROI) calculations are meant to summarize the financial benefits of the program in terms of the reduction in patient health care costs relative to program costs. To that end, the calculations are designed around understanding the costs (relative to each unique patient) prior to entering the program (a.k.a. the baseline period), how those costs change after entry into the program (a.k.a. the measurement period), and ultimately the savings after subtracting the costs for the program itself. A positive ROI is one where the patient costs, after subtracting for the program fees, are less than what they would have been if nothing had changed from the baseline to measurement periods.
ROI Inclusion Criteria
The following logic was applied in creating the ROI measurements through the remainder of this document:
- Patient must have consented to and received treatment in the PHB program.
- Patient had at least six months of eligibility in the baseline and measurement periods.
Time Period: November 2, 2013 through May 31, 2015
Calculation Information:
- Pharmacy costs are excluded per industry standard approaches.
- No other exclusions are applied.
ROI Study #1
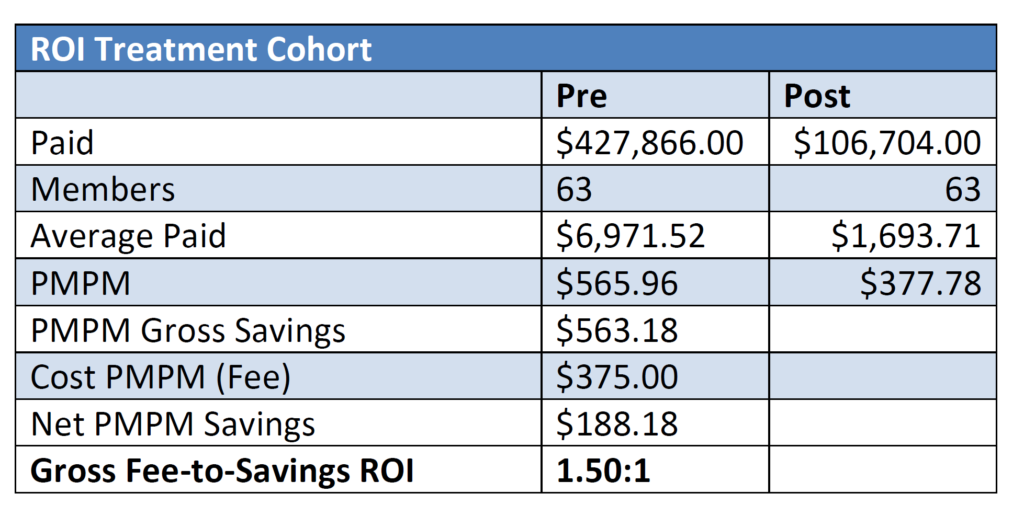
This study compares a 12-month baseline to a preliminary partial period of utilization/costs post-treatment initiation date for each unique patient and then aggregated to the cohort level.
Cohort Selection
- N=63
- Measurement Period
- Pre Period: November 2, 2013 through November 1, 2014
- Post Period: November 1, 2014 through May 31, 2015
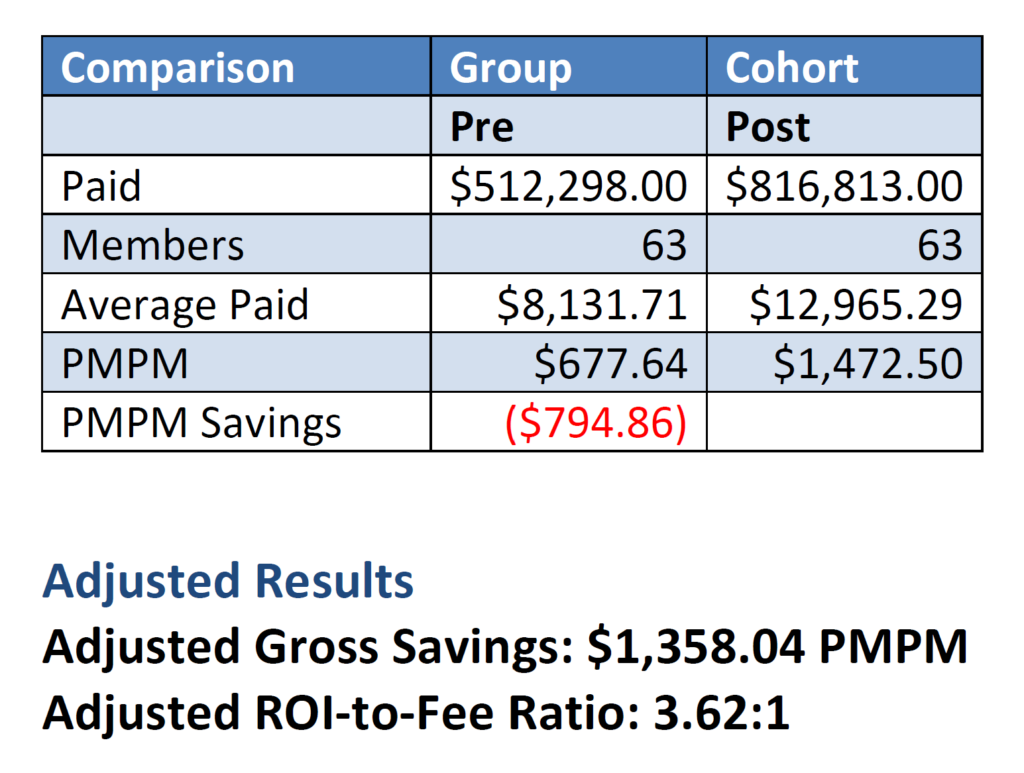
Comparison Group Analysis
Comparison Group: This analysis compares a 12-month baseline to a preliminary partial period of utilization/costs post member identification date for each unique patient targeted but not treated. These calculations are completed for each unique potential patient and then aggregated to the cohort level.
Cohort Selection
- N=63
- Measurement Period o Pre Period: November 2, 2013 through November 1, 2014
- Post Period: November 1, 2014 through May 31, 2015
- Members were matched with ROI cohort members using the following variables:
- Age
- Gender
- Diagnosis
- Pre-period cost parameters
- Identification date